A potential super-antibiotic for super-bugs like MRSA
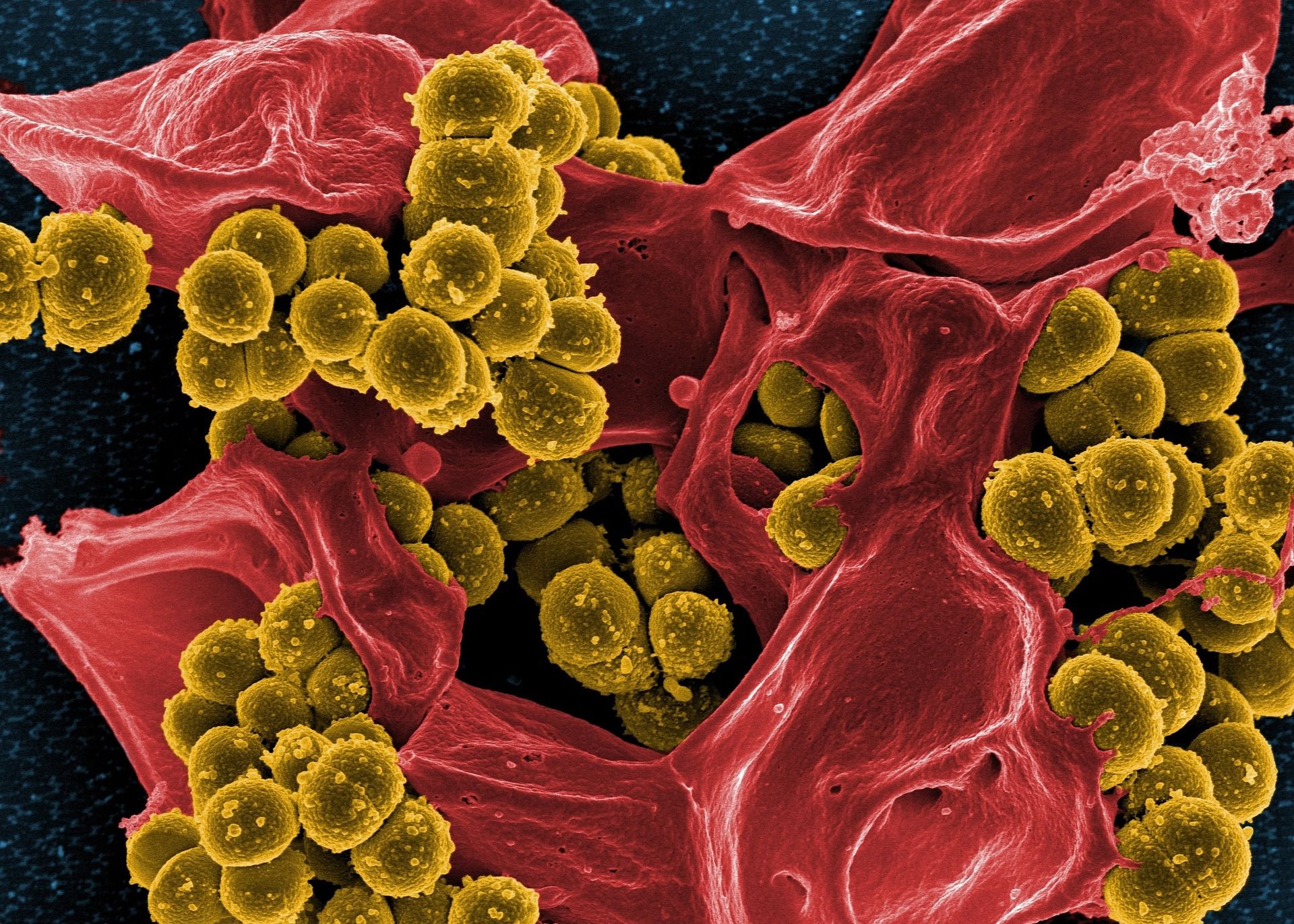
The discovery of a new class of antibiotics, able to kill persistent infections of the “super-bug” methicillin-resistant Staphylococcus aureus (MRSA), provides promise to put us ahead in the arms race against antibiotic resistance.
Each year, the incidence of bacterial infections no longer responding to routine antibiotics increases. As conventional antibiotics are no longer effective in the treatment of infections caused by such bacteria, novel antibacterial therapies are urgently needed.
With the increase of antibiotic-resistant bacteria comes the increase in the number of bacterial strains which cause chronic or recurrent infections, especially if they are able to form non-growing, dormant subpopulations, which are more tolerant to antibiotics. England’s Chief Medical Officer, Dame Sally Davies, alerts us that antibiotic resistance could spell “the end of modern medicine”, due to the impossibility of performing routine operations or defending against simple infections because doctors may run out of antibiotics to keep common infections at bay. It’s this concern that drives the race against time to discover new antibiotics to defend our bodies against infection.
England’s Chief Medical Officer, Dame Sally Davies, alerts us that antibiotic resistance could spell “the end of modern medicine”
New research revolved around the small but significant group of recurrent bacterial infections caused by MRSA. MRSA bacteria are able to evade the immune system, the natural defence system our bodies employ against infection. They do this by the formation of biofilm, which is composed of dormant populations, on medical implants and on the surfaces of wounds. MRSA is also able to thwart the cells involved in the immune response against it, including neutrophils, macrophages, T-cells, and B-cells.
The scientists at Rhode Island Hospital in Providence tested approximately 82,000 small synthetic molecules on MRSA-infected nematodes. Of these, a promising 185 compounds that significantly decreased the ability of MRSA to kill the nematodes were identified. Two of these synthetic retinoids, CD437 and CD1530, were then selected for further testing due to the promise they held. These tests revealed that these two compounds worked by killing both growing and dormant, or “persister”, MRSA cells by disrupting the lipid bilayers which envelope the bacterial cells. Disruptions in this important structure lead to the dysregulation in which compounds enter or leave the cell, thus eventually causing the destruction of a cell.
A promising 185 compounds that significantly decreased the ability of MRSA to kill the nematodes were identified
Modified versions of the synthetic retinoids, either alone or combined with gentamicin (an existing antibiotic), were found to retain anti-persister activity and show an improved cytotoxicity profile, demonstrating considerable efficacy in a mouse model of chronic MRSA infection with no apparent side-effects.
This research holds great promise for the future of antibiotic resistance. With further development and optimization, synthetic retinoids have the potential to become a new class of antibiotics for the treatment of bacterial infections that are currently difficult to treat.
This research holds great promise for the future of antibiotic resistance
Unfortunately, the drugs were not effective against an entire group of pathogens. Urinary tract infections, stomach bugs, gonorrhoea, pneumonia, and the plague, among other diseases, are caused by pathogens which include Escherichia coli, Pseudomonas aeruginosa, Neisseria gonorrhoeae, Klebsiella pneumoniae and Yersinia pestis. It is against these numerous pathogens that the drugs were not effective while proving success against MRSA. This is due to the inherent nature of S. aureus compared to other bacteria, in which their entire biology differs by the absence or presence of an outer-membrane structure. This makes bacteria like E. coli and N. gonorrhoeae, that do have this outer membrane, far less susceptible to antibiotics.
However, the drug does hold great promise for treating chronic MRSA infections that can be lethal for those affected. The lead scientist on the study, Eleftherios Mylonakis, explained that the drug was some years away from human trials, but said that he hopes “that we are a step closer to finding a treatment for the most difficult bacteria”.
The drug does hold great promise for treating chronic MRSA infections that can be lethal for those affected
The fear is that bacteria evolve and develop antibiotic resistance far faster than scientists can develop antibiotics and feasibly distribute them cheaply enough. Health officials have urged that antibiotics be used far more sparingly than that in the past, limiting the opportunity for antibiotic-resistance to evolve in bacterial species, but with antibiotic use having increased by more than 65% since 2000, it seems unlikely that this will happen anytime soon. In an era where the development of antibiotics is struggling to keep pace with the spread of resistant bacteria, the identification of drugs such as these could help researchers to advance a few steps in the arms-race against infectious bacterial disease.
Comments